Preventing type 2 diabetes with better sleep
Would treating sleep apnea—thereby restoring better sleep quality—prevent or delay the onset of type 2 diabetes?
That's what Esra Tasali, MD, Assistant Professor of Pulmonary and Critical Care Medicine at the University of Chicago, hopes to demonstrate through a two-year $1 million study funded by the National Institutes of Health. "If our hypothesis is correct, this study would significantly improve the lives millions of pre-diabetic and diabetic Americans," Tasali said.
Sleep apnea is a disorder characterized by brief recurrent pauses in breathing that disrupt sleep quality. It can cause fragmented sleep that prevents a person from getting sufficient deep sleep, the stage that is thought to be the most restorative.
Diabetes is increasing in epidemic proportions, and the cardiovascular problems that often result from it are the leading cause of death for diabetics. The direct costs of treating diabetes in 2008 were $116 billion; treating the cardiovascular complications associated with diabetes, such as hypertension, cost another $300 billion.
"Despite the demonstrated efficacy of lifestyle interventions and the availability of many drug treatments, the economic and public health burden of diabetes remains enormous," Tasali said. "We aim to alleviate that."
Sleep on it
Nearly 50 million pre-diabetics and diabetics have untreated sleep apnea. Most people with the condition are unaware they have it. Current evidence suggests that sleep apnea increases the risk for cardiovascular disease and may decrease the ability to regulate blood sugar levels, hence increasing the risk of diabetes.
One treatment option is continuous positive airway pressure (CPAP), which uses a machine to deliver a steady stream of compressed air to a patient’s breathing tract via a hose attached to a facemask. The flow of air keeps the airway open thereby preventing breathing interruptions that disturb sleep.
In 2008, Tasali and colleagues published research demonstrating for the first time that lack of deep sleep may increase the risk of type 2 diabetes. The researchers found that suppressing deep sleep by sounds (similar to the sleep fragmentation that would occur with sleep apnea) in healthy young adults significantly decreases their ability to regulate blood sugar levels. After just three nights of deep sleep suppression, the subjects became less sensitive to insulin comparable to that caused by gaining 20 to 30 pounds.
These findings demonstrated a clear role for deep sleep in maintaining normal glucose control. Now Tasali wants to take the next step: to determine whether restoring deep sleep by treating sleep apnea would help pre-diabetics decrease their risk of type 2 diabetes and lower their blood pressure.
In this randomized controlled study, 50 pre-diabetics with sleep apnea will be treated in a sleep lab for 14 consecutive nights with either CPAP or oral medication. The subjects will be overweight or obese and middle aged or older.
Before and at the end of the treatment period, researchers will test the subjects for glucose tolerance, insulin secretion and insulin resistance, all markers for the risk of diabetes. They will also monitor how much the subjects sleep and what kind of sleep they get, as well as their blood pressure, heart rate, weight, energy expenditure and hormones affecting diabetes risk.
If this initial "proof of concept" study is successful, it will provide essential information for designing large multicenter clinical trials that will determine whether treatment of sleep apnea could be a first line intervention to prevent or delay type 2 diabetes—or to improve glycemic control in patients who already have type 2 diabetes, according to Tasali.
"This work has the potential to initiate a major reassessment of clinical recommendations for the prevention, delay and management of diabetes and its cardiovascular complications for millions of Americans," she said.
by Greg Borzo
This award is funded under the American Recovery and Reinvestment Act of 2009, NIH Award number: 3R01HL086459-03S1. For more information on NIH’s Recovery Act projects, visit http://recovery.nih.gov/.
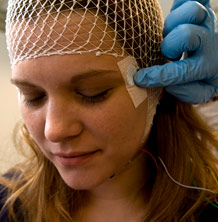
Sleep technologist Harry Whitmore places electrooculogram (EOG) leads for the measurement of eye movements during sleep and wakefulness on participant. Photo by Lloyd DeGrane.










